Utilizing A Home Delivery Pharmacy for Workers’ Comp Savings

Carlisle Medical provides Medical Equipment to assist our patients with a safer and better quality of life:
The average Rx expense is approximately 45% to 50% of annual medical costs for active claims older than ten years. In 2014, Rx prices also saw an inflation rate higher than the overall rate in medical pricing [1]. These cost increases are causing payers to face an important initiative to further reduce pharmacy expenses. Home Delivery Pharmacy service is a worthwhile solution to providing more cost control benefits to payers than a retail pharmacy can provide. These savings come from industry specific clinical staff, lower ingredient costs, lower dispensing fees, medication compliance, and the elimination of mileage costs. While cost savings are crucial to payers, home delivery also provides a unique set of benefits to claimants that include better customer service and the convenience of having medications delivered directly to their home.

Cost Savings Opportunities
Analysis done in recent years by the Centers for Medicare and Medicaid Services (CMS) found that mail-service prescription costs are an average of 16% lower than the same prescriptions filled at retail pharmacies [2].
Work Comp Focus
A workers’ compensation focused clinical pharmacy team can make a significant difference in utilization management. Pharmacists and technicians in this environment are experts with medications that are utilized in the workers’ compensation industry. This familiarity allows pharmacists to alert insurance adjusters about treatment alternatives that may not occur with a non-workers’ comp experienced pharmacy. During the normal filling process, a home delivery pharmacist may also recommend a further in depth clinical Prescription Review of the claimant’s treatment for a potential nurse-physician consult. These value-added features are very powerful and result in real cost savings for payers.
Home Delivery Specialization
A number of different factors help keep medication prices lower in home delivery. Workers’ compensation (WC) home delivery pharmacies are “closed door,” which means they service a particular population without a retail storefront. No storefront means less overhead. Home delivery pharmacies are generally filling a high volume of prescriptions, which allows utilization of technology via robotic automation. This reduces labor and lowers inventory costs through bulk purchasing. A 90-day supply of medication can eliminate the dispense fees associated with the two additional 30-day fills.
Reduction of Out-Of-Network Bills
Out-of-network bills have a large impact on rising pharmacy costs in workers compensation. In many cases, retail pharmacies that receive rejects on a medication fill will attempt to bill through a third party in order to capture the revenue. Trusted home delivery pharmacy partners that are work comp focused do not engage in filling medication without adjuster approval.
Given the right home delivery program, these different methods can be put in place to provide significant savings.
Mileage Reduction
Additional cost savings can come from a reduction in mileage that is paid in almost all states. The reimbursement rate varies by state, but is very close to the national average rate of $.5335 for 2017. (See map below for current state policy on mileage reimbursement.)
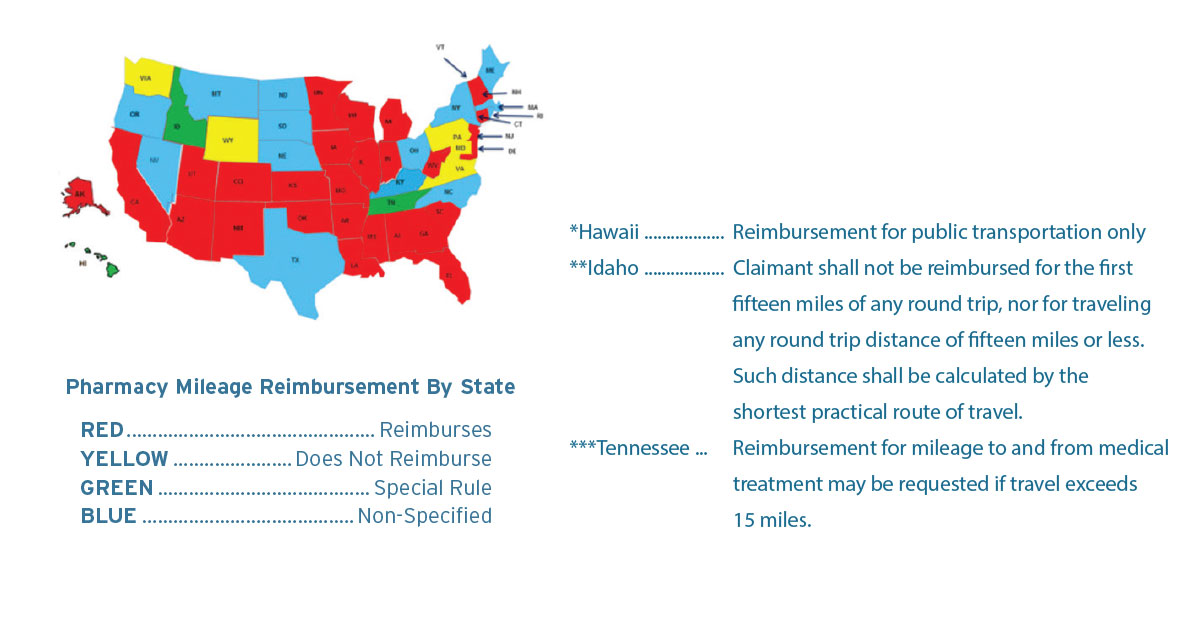
Determining The Right Fit
Determining the best candidates for home delivery requires a continuous review of each claimant’s ever-changing prescribed medications and approval from an insurance adjuster. The number one requirement for home delivery is a need for long-term care. Even though the population of the claimants who require long-term care is small, the cost of prescriptions in this category is a higher expense portion of WC claims. The identification of candidates for home delivery is a meticulous process where the retail pharmacy claimants are reviewed by clinical staff on an ongoing basis. The following criteria provides insight on the screening process for home delivery candidates:
- Consistent medication treatment, in foreseeable future, based on medication treatment plan.
- Injury-related maintenance medications (blood pressure, diabetes, blood thinner and respiratory medications).
- Minimum 30-day prescription.
- Claimants living in rural areas (mileage savings).
- Average monthly shipment exceeds $150.
During the setup of a Pharmacy Management Program, claim managers should strongly consider pre-approving their home delivery pharmacy provider to offer these services where appropriate. In many cases, programs are set up where an adjuster must approve home delivery vs. retail on each injured worker. This is more time-consuming and unnecessary when a trustworthy home delivery pharmacy is providing this service.

The Claimant’s Viewpoint
Convenience and customer service are the most common benefits that draw claimants to a home delivery pharmacy service offering. Claimants benefit from the convenience of having prescriptions shipped directly to their home without requiring a drive to the pharmacy, standing in line, and waiting for prescriptions to be filled. In recent years, advances in technology have made home delivery more convenient for claimants. In the past, state and federal laws required original paper prescription for narcotics, and this required the mailing of prescriptions which would require extra planning and time. This has shifted drastically in recent years. In 2015, Vermont became the final state to legalize electronic prescribing of controlled substances (EPCS) for all schedules of controlled drugs and New York enacted legislation to mandate the use of electronic prescribing for all medications. These shifting dynamics are driving a sharp increase in adoption and utilization of e-prescribing for controlled substances nationwide. In some cases, just getting to the pharmacy itself can be a big challenge, especially if the claimant is homebound. Claimants who live in rural areas can also avoid long drives into the city and find delivery to their home much more convenient. All of these reasons relate back to one basic principal: convenience.
Success Stories
When the customer transitioned to Home Delivery Pharmacy Service they realized a savings of $19,200 over a five-year period.
SUCCESS STORY 1: During a recent customer service encounter, a staff member recognized that a claimant was filling their prescriptions for a long-term injury through retail service. The claimant was contacted and convinced to take advantage of the home delivery service. The claimant has since experienced a better and more convenient service and the payer received savings. When transitioned to Home Delivery Pharmacy Service, 25% savings was realized on five medications for the claimant. The annual savings equaled $3,840 or $19,200 over a five-year period. Home Delivery Pharmacy staff are highly trained and available to assist in efforts to transition claimants to their service.

By utilizing home delivery, a customer avoided an unnecessary expense of $75 a month in mileage reimbursement.
SUCCESS STORY 2: During a recent customer service encounter, a retail customer service representative determined in conversation that a claimant was traveling 70 miles round trip from their house to their pharmacy. This claimant was convinced to utilize home delivery and was happy to avoid the long drive. By the claimant utilizing home delivery, the payer avoided the unnecessary $75 a month in mileage reimbursement. Home Delivery Pharmacies have the ability to offer increased savings over Retail Pharmacy programs.

IN CONCLUSION
Companies can definitely gain a positive return on investment from home delivery pharmacy services. In our experience, many companies have the potential to save an average of 16% on dollars by partnering with a workers’ compensation home delivery pharmacy.
ADDITIONAL RESOURCES:
This white paper was prepared by Jeff Carlisle, Assistant Vice President for Carlisle Medical, in collaboration with staff and pharmacists. Carlisle Medical has more than 35 years of experience as a leader in health care cost containment in the workers’ compensation industry. Our company assists insurance carriers, third-party administrators, and employers significantly reduce their workers’ compensation costs. Our experienced staff of licensed pharmacists and nurses can assist companies with injuries ranging from minor to catastrophic.
REFERENCES:
[1] Workers Compensation and Prescription Drugs: 2016 Update – May 5, 2016
[2] Part D Claims Analysis: Negotiated Pricing between General Mail Order and Retail Pharmacies